Uterovaginal prolapse occurs when the uterus and/or vaginal walls drop from their normal position into the vaginal canal due to weakened pelvic floor muscles and ligaments. This can happen due to childbirth, ageing, or other factors that affect the pelvic support system. Uterovaginal prolapse is a common condition, especially among women who have given birth multiple times or gone through menopause.
Uterovaginal prolapse can present with a variety of symptoms, ranging from mild discomfort to more noticeable physical changes. Common symptoms include:
Especially in the pelvic region or lower back.
Some women may feel or see a bulge of tissue protruding from the vaginal opening.
Trouble starting urination, frequent urination, or feeling like you can’t completely empty your bladder.
Difficulty with bowel movements or the sensation of incomplete emptying.
Uterovaginal prolapse can cause discomfort or pain during sexual activity.
Some women may experience irregular bleeding or increased vaginal discharge.

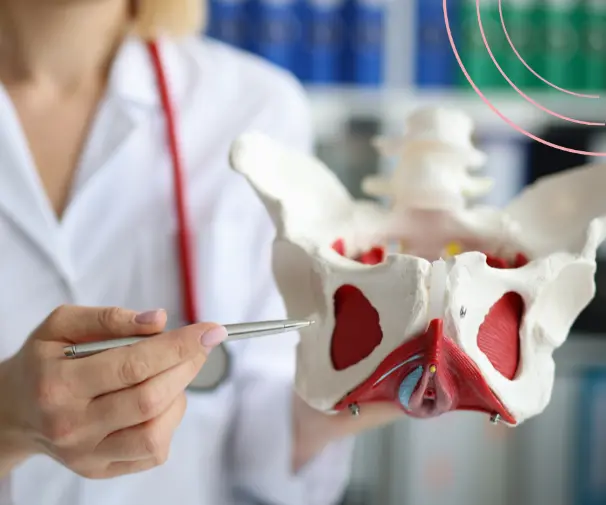
Uterovaginal prolapse occurs when the pelvic floor muscles and ligaments become weakened, often due to a combination of factors. Childbirth, particularly after multiple vaginal deliveries or delivering large babies, can strain these muscles. Ageing and menopause also play a role, as the natural decline in oestrogen levels can weaken pelvic tissues over time. Chronic pressure from conditions such as persistent coughing, constipation, or heavy lifting further increases the strain on pelvic organs. Additionally, obesity can contribute by placing extra stress on the pelvic floor, while some women may have a genetic predisposition to prolapse due to inherited tissue weakness.
A comprehensive approach is required to diagnose uterovaginal prolapse. This includes:

A rectocele prolapse occurs when the wall between the rectum and the vagina weakens, causing the rectum to bulge into the vaginal wall. This can create discomfort, a feeling of heaviness, or difficulty with bowel movements. For many women, it’s a condition that can affect daily life, but it’s also a topic many feel hesitant to discuss.
The symptoms of rectocele prolapse can vary but may include:
While these symptoms can be distressing, they are treatable with the right approach.
Dr. Orla Conlon and her team are dedicated to providing expert care for women with any type of prolapse. They understand the sensitive nature of this condition and create a safe, supportive environment where women feel heard and cared for.
We offer a wide range of treatment options tailored to your specific needs, including:

Advice on exercises such as pelvic floor strengthening (Kegels) to help improve muscle tone and support.

Oestrogen replacement therapy may be recommended for postmenopausal women to strengthen the pelvic tissues.
A non-surgical option where a silicone device is inserted into the vagina to support the uterus and relieve symptoms.

Surgical repair options such as vaginal or laparoscopic procedures to restore the normal position of the pelvic organs.

We offer surgical options tailored to your needs, including uterine-sparing procedures for those wishing to preserve the uterus and hysterectomy for more severe cases requiring long-term symptom relief.
Treating the whole person, not just the condition, along with medical treatments, consider / ask your specialist about:
Expert-guided exercises and therapies to strengthen the muscles and improve pelvic stability.
Comprehensive care after surgical treatment, including rehabilitation and pelvic therapy to ensure a smooth recovery.
We understand that uterovaginal prolapse can impact your confidence and quality of life, so we provide counselling and support services to help you through your treatment journey.